Patients with advanced chronic kidney disease (CKD) or severe acute kidney injury (AKI) may require dialysis to remove waste and excess fluid from the blood. While many people receive dialysis at a treatment center, some may qualify for home dialysis, including peritoneal dialysis (PD) or home hemodialysis (HHD).
Understanding how these dialysis options work can help patients and families prepare for the next stage of kidney care.
Dialysis Treatment Options
Patients with kidney failure may receive dialysis in several ways depending on their health and lifestyle.
Options typically include:
- In-center hemodialysis performed at a dialysis clinic
- Home hemodialysis using specialized dialysis equipment
- Peritoneal dialysis is performed at home
Each treatment approach has unique advantages, and a nephrologist can help determine which option is most appropriate.
Learn more in our guide to In-Center Hemodialysis.
What Dialysis Does for the Body
Healthy kidneys filter waste, balance fluids, and regulate important minerals in the blood. When kidney function declines significantly, dialysis helps replace some of these functions.
Dialysis helps the body:
- Remove waste products from the blood
- Balance electrolytes, including potassium and sodium
- Remove excess fluid
- Help control fluid balance and blood pressure
Although dialysis does not cure kidney disease, it can help manage symptoms and maintain overall health when the kidneys can no longer perform these essential functions.
When Dialysis May Be Needed
Dialysis may be recommended when the kidneys are no longer able to filter waste and fluids effectively.
Common situations where dialysis may be needed include:
- Advanced chronic kidney disease (usually stage 5 or late stage 4 with symptoms)
- Kidney failure
- Severe acute kidney injury (AKI)
Symptoms of kidney failure may include:
- Swelling in the legs, ankles, or abdomen
- Persistent fatigue or weakness
- Nausea or vomiting
- Fluid retention
- Shortness of breath
Some patients receive dialysis treatments in a specialized clinic.
What Is Home Dialysis?
Home dialysis refers to dialysis treatments performed outside of a dialysis center after patients complete specialized training with their nephrology care team.
Patients may perform dialysis:
- Independently
- With assistance from a caregiver
The two primary types of home dialysis include:
- Home Hemodialysis (HHD)
- Peritoneal Dialysis (PD)
Compared with dialysis performed in a treatment center, home dialysis may involve:
- Shorter or more frequent treatments
- Flexible scheduling
- Greater patient participation in care
- Caregiver involvement when needed
Some patients prefer home dialysis because it allows them to receive treatment in their own environment while maintaining greater control over their daily routine.
Types of Home Dialysis
Home Hemodialysis (HHD)
Home hemodialysis works similarly to dialysis performed in a clinic but uses a dialysis machine designed for home use.
During treatment:
- Blood is removed from the body through a vascular access. Home hemodialysis typically uses vascular access such as an arteriovenous fistula (AV fistula), arteriovenous graft, or dialysis catheter.
- The blood passes through a dialyzer (artificial kidney).
- Waste products and excess fluid are removed.
- Cleaned blood returns to the body.
Typical characteristics of home hemodialysis include:
- Performed at home
- Uses a home dialysis machine
- Treatments may occur 3–5 times per week, though some patients perform shorter daily treatments or overnight dialysis depending on their care plan.
- Sessions usually last 3–4 hours
Some patients perform shorter treatments more frequently or overnight depending on their care plan.
Peritoneal Dialysis (PD)
Peritoneal dialysis uses the peritoneal membrane — a thin lining inside the abdomen — as a natural filter to remove waste products and excess fluid from the blood.
A soft catheter placed in the abdomen allows dialysis fluid to move in and out of the abdominal cavity.
Typical characteristics include:
- Performed at home
- Uses the body’s peritoneal membrane for filtration
- Usually performed daily
Because dialysis exchanges occur regularly throughout the day or overnight, many patients find peritoneal dialysis fits well into their lifestyle.
How Peritoneal Dialysis Works
The process typically includes several steps:
- Dialysis fluid enters the abdomen through a catheter.
- The peritoneal membrane acts as a filter.
- Waste products and excess fluid move from the blood into the dialysis solution.
- The fluid containing toxins is drained and replaced with fresh solution.
This process is called an exchange.
Each exchange allows the body to remove waste products gradually throughout the day or night.
Types of Peritoneal Dialysis
Continuous Ambulatory Peritoneal Dialysis (CAPD)
CAPD is performed manually during the day.
Characteristics include:
- Manual fluid exchanges
- Typically 3–5 exchanges per day
- No machine required
Patients perform exchanges at scheduled intervals throughout the day.
Automated Peritoneal Dialysis (APD)
Automated peritoneal dialysis uses a cycler machine to perform fluid exchanges overnight while the patient sleeps.
Typical features include:
- Use of a dialysis cycler machine connected to the catheter
- Treatment performed at home
- Minimal interruption to daytime activities
One common form of APD is continuous cycling peritoneal dialysis (CCPD), in which the cycler performs several exchanges overnight, and dialysis fluid may remain in the abdomen during the day between treatments.
Peritoneal Dialysis Catheter Placement
Before starting peritoneal dialysis, a catheter must be surgically placed in the abdomen.
This process typically includes:
- A minor surgical procedure
- Placement of a flexible catheter
- A healing period before dialysis begins
- Training with dialysis nurses
Proper catheter care is important to reduce infection risk and maintain effective dialysis treatments.
Common Experiences with Peritoneal Dialysis
Each patient’s experience with dialysis can vary. However, some physical sensations are common when beginning peritoneal dialysis.
Why Peritoneal Dialysis Can Cause a Swollen or Bloated Belly
Many patients notice a feeling of abdominal fullness during treatment.
Mild bloating is common early in treatment as the body adjusts to dialysis fluid volumes. This occurs because dialysis fluid fills the abdominal cavity while filtering the blood. Patients may notice:
- A temporary increase in waist size
- Mild abdominal pressure
- A feeling of fullness
After the dialysis fluid drains, the abdomen typically returns to its usual size.
Tips Patients Share for Managing PD Bloating
Patients often use several strategies to reduce discomfort during peritoneal dialysis:
- Wearing loose or comfortable clothing
- Adjusting dialysis fluid volumes
- Performing overnight exchanges
- Maintaining regular physical activity
- Working closely with the dialysis care team
A nephrology team can help adjust treatment settings if symptoms persist.
Possible Risks of Peritoneal Dialysis
Although many patients tolerate peritoneal dialysis well, complications can occur.
Possible risks include:
- Peritonitis (infection of the abdominal lining)
- Catheter infections
- Hernias
- Inadequate dialysis in some patients
- Weight gain from glucose-based dialysis fluid
Dialysis teams provide training and infection-prevention education to help reduce these risks.
Home Dialysis vs In-Center Dialysis
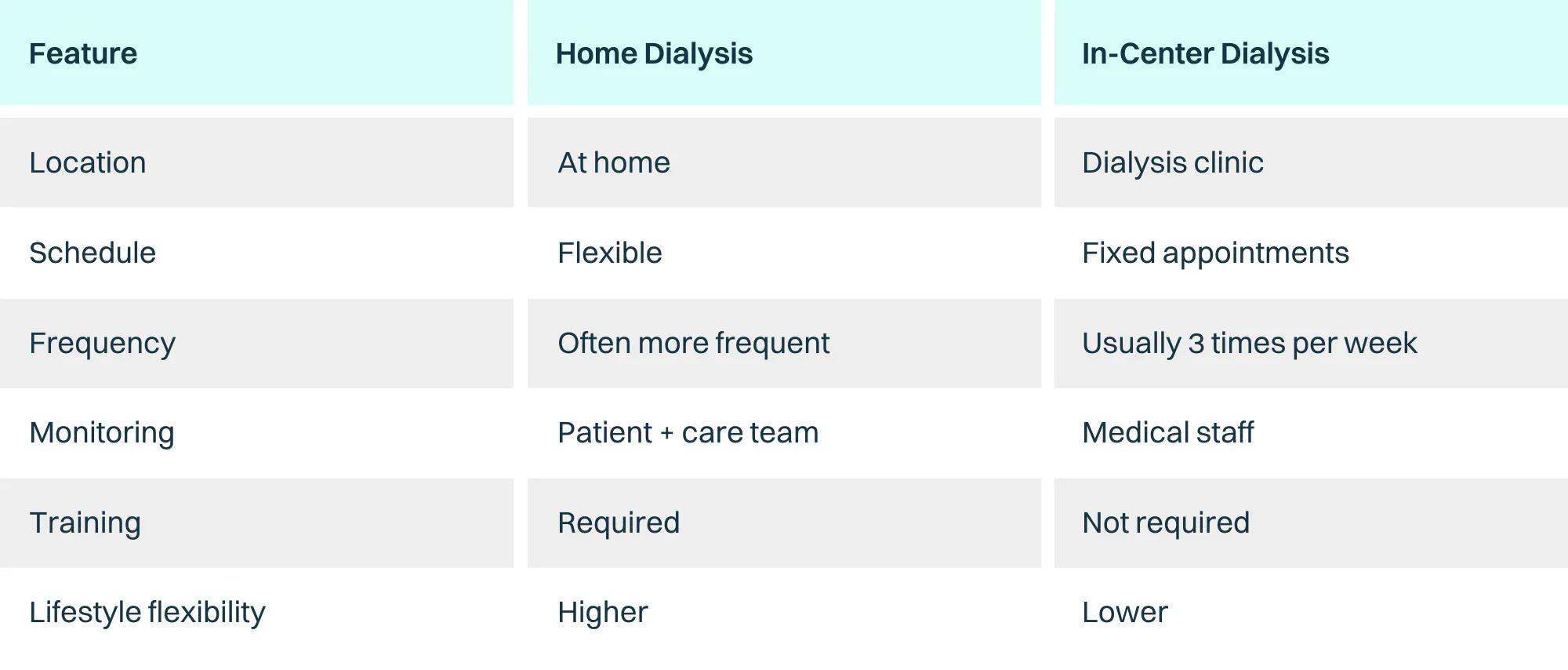
Each dialysis option has advantages and limitations, and a nephrology care team can help determine which approach is most appropriate for each patient.
Advantages of Home Dialysis
Home dialysis may offer several benefits for some patients, including:
- Flexible treatment schedules
- Fewer trips to dialysis centers
- Overnight dialysis options
- Greater independence and control
Many patients appreciate the ability to integrate dialysis treatments into their daily routines.
Potential Challenges of Home Dialysis
Despite its advantages, home dialysis may also present challenges.
Possible challenges include:
- Training requirements
- Risk of infection
- Catheter care responsibilities
- Equipment storage
- Abdominal discomfort with peritoneal dialysis
A nephrology team helps patients determine whether home dialysis is a safe and appropriate option.
What Daily Life Can Look Like on Home Dialysis
Starting dialysis can feel overwhelming, but many patients continue to work, travel, and maintain active lives while receiving home dialysis.
Patients often ask about:
- Managing work schedules
- Traveling with dialysis equipment
- Diet and fluid restrictions
- Exercise and activity levels
With training and support from a nephrology team, many people successfully integrate dialysis treatments into their everyday routines.
Diet and Fluid Changes on Dialysis
Dialysis patients often need to adjust their diet and fluid intake to maintain healthy electrolyte and fluid balance.
Common dietary considerations include:
- Limiting sodium to control blood pressure and fluid retention
- Managing potassium levels
- Monitoring phosphorus intake
- Maintaining adequate protein intake to replace protein lost during dialysis
Fluid intake may also need to be monitored depending on the type of dialysis and remaining kidney function.
A nephrologist or renal dietitian can help create an individualized diet plan that supports dialysis treatment and overall health.
Who May Be a Candidate for Home Dialysis
Candidates for home dialysis may include:
- Patients with advanced CKD (stage 4–5)
- Individuals motivated to manage treatments at home
- Patients with caregiver support when needed
- Individuals approved by a nephrologist
A full medical evaluation is necessary before starting any dialysis program.
How Long Can Someone Live on Home Dialysis?
Many people live for years while receiving dialysis treatment. Survival depends on several factors, including overall health, age, underlying kidney disease, and how well dialysis treatments are managed.
Some patients remain on dialysis long term, while others may eventually receive a kidney transplant. For eligible patients, kidney transplantation often offers improved long-term survival and quality of life compared with dialysis alone.
Working closely with a nephrology team, maintaining a healthy lifestyle, and following dialysis instructions can help improve quality of life and long-term outcomes.
Is Home Dialysis Better Than In-Center Dialysis?
The best dialysis option depends on several factors, including:
- A patient’s medical condition
- Lifestyle and work schedule
- Support system
- comfort with managing treatments
Some patients prefer home dialysis because it offers flexibility and independence. Others prefer in-center dialysis, where medical staff perform treatments.
A nephrologist can help determine which dialysis option is most appropriate.
FAQs
Peritoneal dialysis is a type of dialysis that uses the lining of the abdomen (peritoneal membrane) to filter waste and excess fluid from the blood.
Dialysis fluid enters the abdomen through a catheter, absorbs waste and fluid through the peritoneal membrane, and is then drained and replaced with fresh solution.
Yes. Peritoneal dialysis is typically performed at home after training with a dialysis care team.
Possible disadvantages include infection risk, equipment storage needs, training requirements, and the need to manage treatments regularly.
Hemodialysis filters blood through an external dialysis machine, while peritoneal dialysis uses the body’s abdominal lining as a natural filter.
Dialysis fluid temporarily fills the abdomen during treatment, which can create a feeling of fullness or mild bloating. The sensation usually improves after the fluid drains.
When to Talk to a Nephrologist About Dialysis
Patients should speak with a kidney specialist if they experience:
- Worsening kidney function
- Swelling or fluid buildup
- Persistent fatigue
- Abnormal kidney test results
Early discussions with a nephrologist can help patients plan dialysis options and prepare for treatment if needed.
Schedule a Dialysis Consultation
If you have advanced kidney disease or symptoms of kidney failure, a nephrologist can help you understand your dialysis options, including home dialysis and in-center treatments.
Schedule a consultation with a nephrologist to discuss the best dialysis approach for your health and lifestyle.
